Coronavirus Update
Dear Patient,
At FORM Ortho, the safety and welfare of our patients and staff are our number one priority. We have been continually reviewing CDC recommendations and updating our preventive and responsive actions accordingly. In an effort to continue to provide care to those that need it, while also keeping the health of our patients and staff a priority, we wanted to update you on some adjustments we have made within our practice during this unprecedented time.
- As per multiple guidelines, we have greatly enhanced our disinfecting techniques.
- We have complied whenever possible with social distancing guidelines.
- FORM Ortho will remain open and will be treating patients. We’re offering this service to help patients avoid crowded waiting rooms in urgent care centers and emergency rooms.
- We are rigorously screening staff and patients on an ongoing basis so that those with any risk factors for COVID19 are given the opportunity to reschedule or participate in a telemedicine visit if appropriate.
We urge you to stay home if you are sick and continue to practice good hand hygiene, and cover coughs.
If you are sick and/or have a fever, cough, or shortness of breath, contact your primary care provider immediately. If you have any of these symptoms, we also ask you to call our office to reschedule your appointment.
To get started with your FORM Ortho appointment, please call (510) 857-1000 to schedule or you may request an appointment online.
As CDC recommendations are updated, we will make adjustments accordingly. Likewise, we will do the same for any local and state health department directives to ensure the continued safety of our patients.
Sincerely,
Basil R. Besh, MD
Meet Our Doctor

Basil R. Besh, M.D.
The mission of FORM Ortho is to be the preferred provider of orthopedic care and occupational health amongst our community, case managers and primary care physicians. We believe in earning the trust of our patients, not only by providing the highest quality and leading-edge medical care but also by treating each patient and their family with sincere compassion. The ultimate goal of our entire organization is to aid and support each patient as they navigate the healthcare process, which can be very stressful.
Meet Our Doctors
Check Out Our Patient Reviews
The MostCommon Injuries
Injuries disrupt life. Significant injuries can happen without warning at work, at home or while playing sports.
Need Help Now?
Work-Related
Hurt on the job? It’s important to report it to your employer right away, and seek treatment as soon as possible.
> Read More
Sports-Related
Don’t let a sports injury interrupt the game or your life.
> Read More
Home-Related
Falls are the number one cause of home injuries in the U.S.
> Read More
Restore motion and reduce pain.
Frequently Asked Questions
Orthopedic surgeons are devoted to the prevention, diagnosis, and treatment of disorders of the bones, joints, ligaments, tendons, and muscles.
Some orthopedists are generalists, while others specialize in certain areas of the body, such as:
- Hip and knee
- Foot and ankle
- Shoulder and elbow
- Hand
- Spine
Orthopedic surgeons explore nonsurgical options first, such as pain medication or
rehabilitation. They also have the expertise to perform surgery to repair an injury or
correct a condition, if necessary.
Musculoskeletal pain is the number one reason why people visit their doctors each
year.
To learn about the treatment and management of orthopedic conditions, visit The
American Academy of Orthopaedic Surgeons’ (AAOS) patient education website,
orthoinfo.org.
An orthopedic surgeon is an expert with extensive training in the proper diagnosis and the treatment (both nonsurgical and surgical) of injuries and diseases of the musculoskeletal system.
A qualified hand specialist is trained to diagnose and treat all problems related to the different structures in the hand, wrist, and forearm.
The hand is a unique area of the human body that is made up of bones, joints, ligaments, tendons, muscles, nerves, skin, and blood vessels. These elements must all be in good working order for the hand to function well.
The relationship between all these structures is delicate and refined. An injury or disease can affect any or all of these structures and impair the use of the hand.
Hand specialists have received additional specialized training in the treatment of hand problems. Many also have expertise with problems of the elbow, arm, and shoulder. Some treat only children, some treat only adults, and some treat both. Common problems treated include:
- carpal tunnel syndrome
- tennis elbow
- wrist pain
- sports injuries of the hand and wrist
- fractures of the hand, wrist, and forearm
- trigger finger
Other problems treated can include arthritis, nerve and tendon injuries, and congenital limb differences (birth defects).
Not all problems treated by a hand specialist need surgery. They often recommend nonsurgical treatments, such as medication, splints, therapy, or injections.
If you have pain in your fingers, hand, wrist or arm, or if you have other upper-extremity related concerns, you may want to consult a hand specialist.
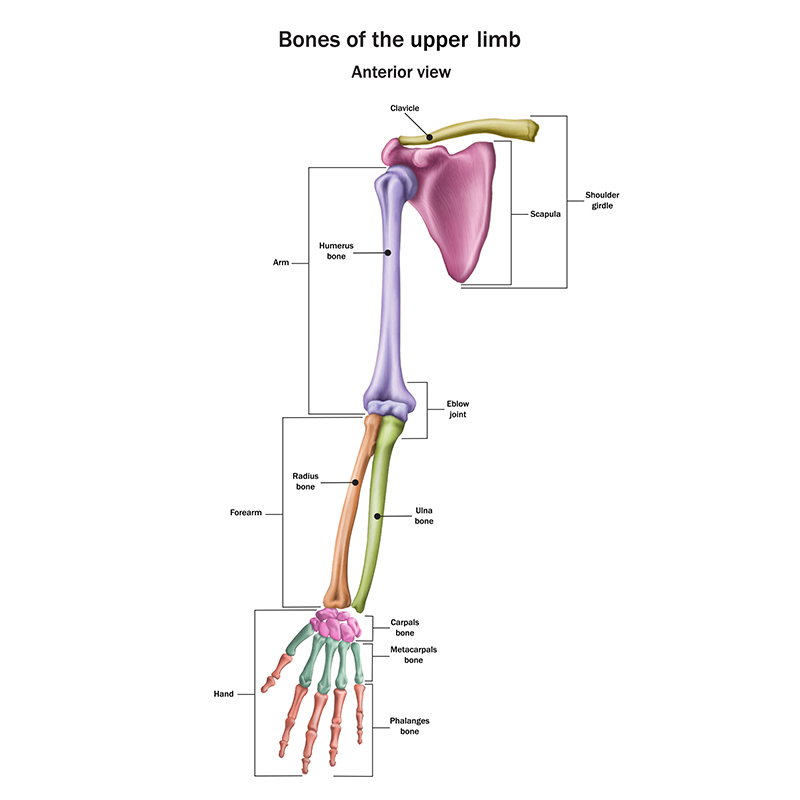
The upper extremity consists of the shoulder, elbow, wrist, and hand. The upper limb is divided into three regions that consist of the arm, located between the shoulder and elbow joints; the forearm, which is between the elbow and wrist joints; and the hand, which is located distal to the wrist.
Dr. Besh is fellowship-trained and a board-certified orthopedic surgeon specializing in Hand, Wrist, and Elbow conditions. He is one of the few hand surgeons in Silicon Valley that has the Subspecialty Certificate in Surgery of the Hand and has over 15 years of experience focused on orthopedic hand conditions.
Dr. Besh is an expert in upper extremity and hand conditions. If you are experiencing pain or discomfort in your hands, fingers, wrist, or elbow, or have additional concerns, contact our office for an appointment.
Occupational Medicine (also known as Occupational Health) is focused on the treatment of work-related injuries and illnesses. Physicians trained in Occupational Medicine diagnose and treat work-related injuries much more effectively than most primary care physicians. They’re up-to-date on federal and state regulations for workforce health and safety, including the Occupational Safety and Health Administration (OHSA), the Department of Transportation (DOT), and the Federal Aviation Administration (FAA), so that they can make the best treatment plans and perform regulatory examinations. Occupational medicine physicians often work directly with employers to keep business running and employees safe and healthy on the job.
FORM Ortho offers a wide range of occupational health services such as post-offer physical exams, drug screening, surveillance testing for OSHA, and many other medical services to support employers and their employees.
At FORM Ortho, we understand the workers’ compensation process and we are set up to report as needed for workers’ compensation claims.
Our team of specialists will provide you with an immediate diagnosis of the injury, corrective treatment, and medication if needed. We’ll also discuss long-term options for recovery.
A sports medicine physician has significant specialized training in both the treatment and prevention of illness and injury. They are ideally suited to provide comprehensive medical care for athletes, sports teams or active individuals who are simply looking to maintain a healthy lifestyle. Sports medicine physicians specialize solely in non-surgical sports medicine and serve as team physicians at the youth level, NCAA, NFL, MLB, NBA, WNBA, MLS, and NHL, as well as with Olympic teams.
A sports medicine physician can maximize non-operative treatment, guide appropriate referrals to physical and occupational therapies, and if necessary, expedite referral to an orthopedic/sports surgeon.
Common examples of musculoskeletal problems include:
- Acute injuries (such as ankle sprains, muscle strains, knee and shoulder injuries, and fractures)
- Overuse injuries (such as rotator cuff and other forms of tendonitis, stress fractures)
- Medical and injection therapies for osteoarthritis
Sports Medicine physicians have also received additional training in the non-musculoskeletal aspects of sports medicine. Common examples of these include:
- Concussion (mild traumatic brain injury) and other head injuries
- Athletes with chronic or acute illness (such as infectious mononucleosis, asthma or diabetes)
- Nutrition, supplements, ergogenic aids, and performance issues
- Exercise prescription for patients who want to increase their fitness
- Injury prevention
- “Return to play” decisions in the sick or injured athlete
- Recommendations on safe strength training and conditioning exercises
- Healthy lifestyle promotion
Our physicians specialize in general orthopedics as well as surgery of the Foot and Ankle, Hand, Wrist, Elbow, Shoulder, and Knee. We also offer Immediate Injury Care for Sports-Related Injuries, Work-Related Injuries, and Home-Related injuries.
Additionally, we have a full-service Occupational Medicine clinic that focuses on work-related injuries and illnesses. We can even assist you with Workers’ Compensation injuries and claims.
For the convenience of our patients, we also offer additional services on-site including:
- Hand Therapy
- Physical Therapy
- Digital X-Ray
- Open MRI
- Precision SurgiCenter (outpatient surgery center)
Load More
Show More
Show Less






